The PIOA Introductory and Trauma modules were held at the Colonial War Memorial (CWM) Hospital in Suva, Fiji from March 4th to 16th, 2024.

Week 1 Back row from L to R, Faculty in bold, Penijamini Naiceru (Fiji) Tzun Rafael (Palau,) James Tewa’ani (Solomon Islands, Pita Sovanivalu (Fiji), Tommy Walters (PNG), Juvencio Dias (Timor Leste), Shaun Mauiliu (Samoa), Manoa Valeniyasana (Fiji),Robert Fa’ataga (Samoa), Jeffrey Yiapi (Solomon Islands), Paul Lomavatu (Fiji). Front row from L to R Jacky Pahun (PNG), Pauliasi Bauleka (Fiji), Oralae Pitakia (Solomon Islands), Viola Kokiva (PNG)
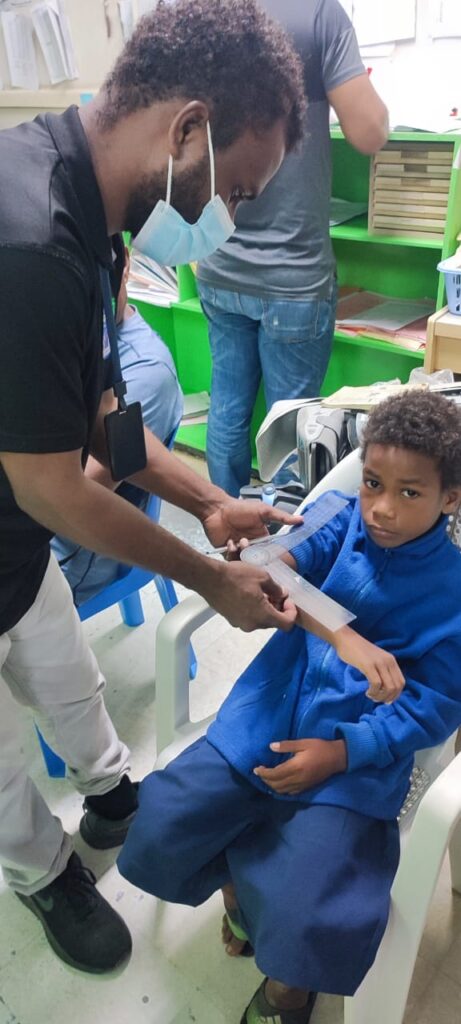
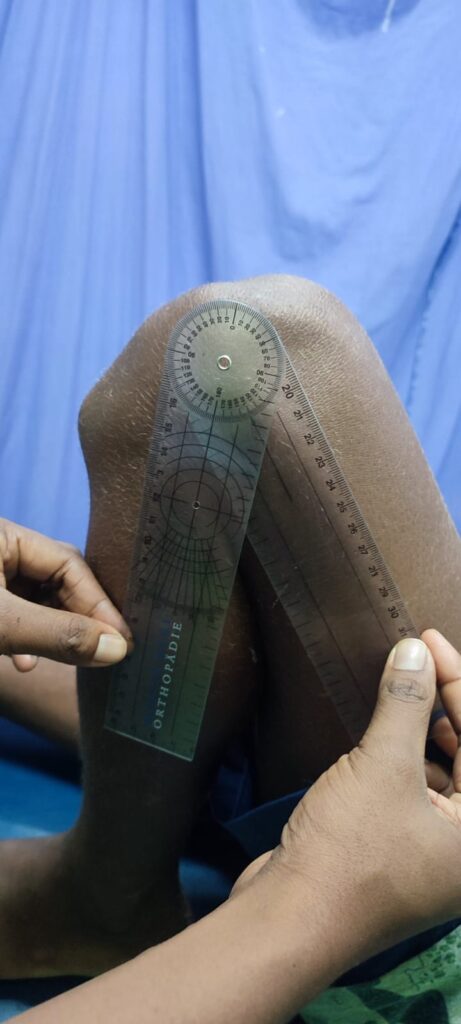
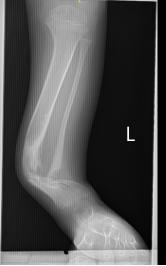
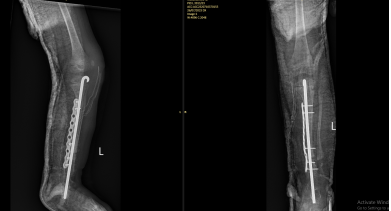
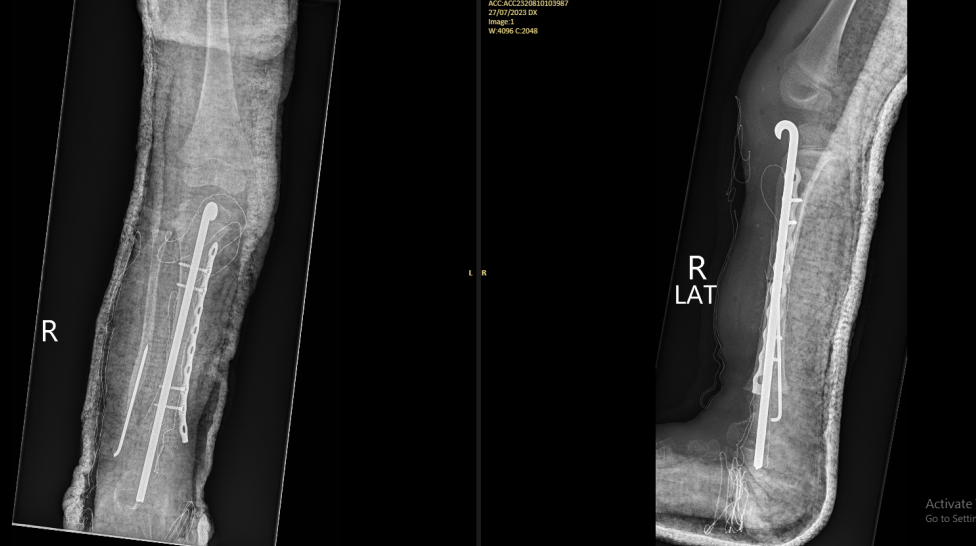
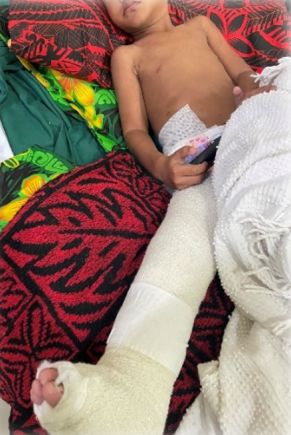
In this module, the students were taught a systematic approach to diagnosis and management of orthopaedic conditions and trauma. This included clinical history taking and a thorough clinical examination, investigation and a structured, systematic approach to orthopaedic decision making. There was also an emphasis on a systematic approach to the management of trauma including the management of the soft tissues and the management of closed and open fractures. In addition, there were focussed lectures and practicals on the management of trauma affecting the long bones of the limbs.

Lectures were supplemented with practical demonstrations. Each morning. we commenced with a ward round seeing two patients and getting the students to present the history and clinical signs of the patients. Their management was then discussed and suggestions for improvement were made. This was a useful exercise as we were able to improve clinical skills. It was also helpful to try and elucidate clinical reasoning and decision making and help with developing these skills. The students enjoyed having expert advice on the diagnosis and management of trauma –which is common condition throughout the Pacific and are often poorly managed. The students were assessed with practical tasks (history taking, focussed clinical examinations and a practical external fixation task as well as a written examination on the final day of the modules.

Week 2 Back row from L to R, , Penijamini Naiceru (Fiji), Tommy Walters (PNG), Haynes Rasin (PNG), Juvencio Dias (Timor Leste), Viola Kokiva (PNG), Jacky Pahun (PNG),Tzun Rafael (Palau,) Jeffrey Yiapi (Solomon Islands) Paul Lomavatu (Fiji), Manoa Valeniyasana (Fiji), Robert Fa’ataga (Samoa), Front row Faculty in bold from L to R Pita Sovanivalu (Fiji), Mark Rokobuli (Fiji), Des Soares (Australia), Areta Samuelu (Samoa), Clay Sios i (Solomon Islands.