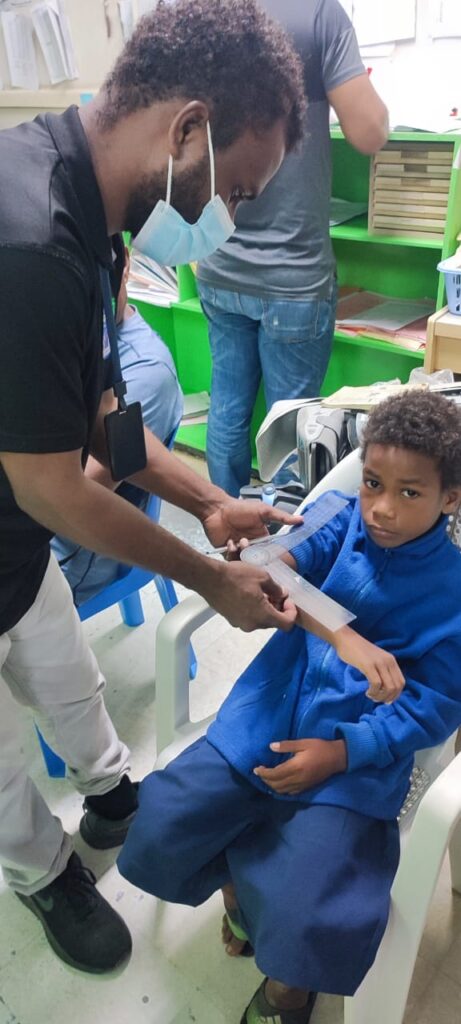
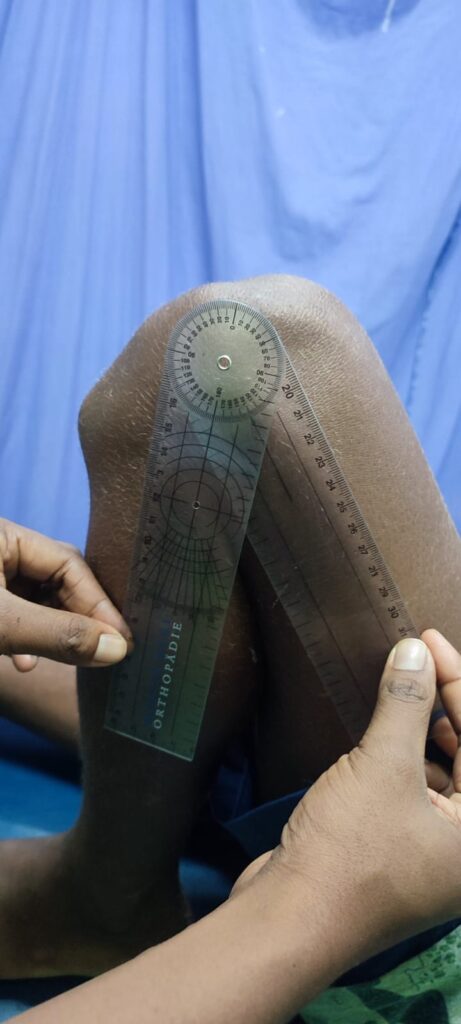
Great to see Dr Agnes Auto, PIOA registrar in Honiara, training the next generation. Learning to use the goniometers gifted by PIOA. Accurate measuring and recording are the basis of good orthopaedic decision making.





Pacific Islands Orthopaedic Association
Bringing quality orthopaedic education to the Pacific Islands
Great to see Dr Agnes Auto, PIOA registrar in Honiara, training the next generation. Learning to use the goniometers gifted by PIOA. Accurate measuring and recording are the basis of good orthopaedic decision making.





PIOA graduate Dr Areta Samuelu was delighted to welcome PIOA lecturers Dr. Tim Gregg from Wellington, NZ and Dr Jason Donovan from Waikato, NZ on a surgical visit. Tim and Jason are experienced paediatric orthoapedic surgeons. The purpose of the visit was to help and train Areta in the management of congenital pseudoarthosis of the tibia, a rare but debilitating condition affecting the lower limb. You can read about the visit in detail below.
Some pictures from the visit.
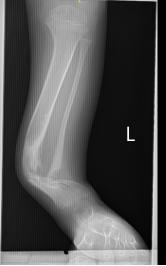
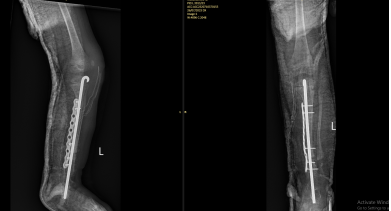
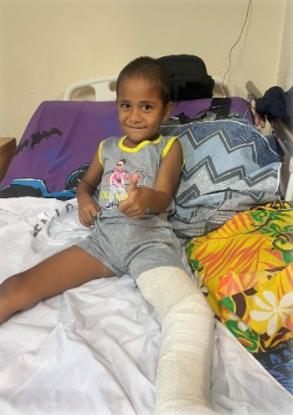
Congenital Pseudoarthrosis of the Tibial- Extremely rare- 1:140,000-190,000- Anterolateral Bowing and Congenital Pseudoarthrosis of the Tibia are congenitalconditions, most commonly associated with Neurofibromatosis Type 1, that present with abowing deformity of the tibial.- Diagnosis is confirmed with radiographs of the tibia.- Treatment is nonoperative with bracing for patients who are weightbearing withoutpseudoarthrosis or fracture. Surgical correction is indicated in the presence ofpseudoarthrosis or fracture.- Risk Factors- Up to 55% associated with Neurofibromatosis Type 115% associated with Fibrous Dysplasia
In planning for both these cases, it took a year for it to fruition. Both cases turned up to our clinic in 2021 and then the whole of 2022- 2023 took time for us to plan around covid and especially counselling for the parents in both these cases as both cases will need follow up till these kids reach skeletal maturity as both cases are very rare and only a few people can do this operation.With the use of our network in both NZ and Australia, we reach out for help, and we develop a discussion and options for both patients, In March 2023, they visited Samoa as course convenors for the PIOA Paediatric Module. This great opportunity was considered also to discuss and ask for their advice on the complex paediatric cases we had on island.Dr.Tim Gregg and Dr.Jason Donovan are both renowned consultant orthopedic surgeons working in Wellington and Waikato NZ respectively. They specialize in Pediatric orthopedics and are facilitators / Mentors for the PIOA (Pacific Island Orthopedic Association) program in the Pacific and are integral part of the training program for NZ trained orthopedic surgeons.Following this meeting, both surgeons then made their own arrangements by volunteering freely and own funding through the PIOA collaboration to aid and management of our complex cases.As part of our planning phase, we had the privilege of having one of the reps from NZ to assist us with the equipment’s from Paragon Medical.
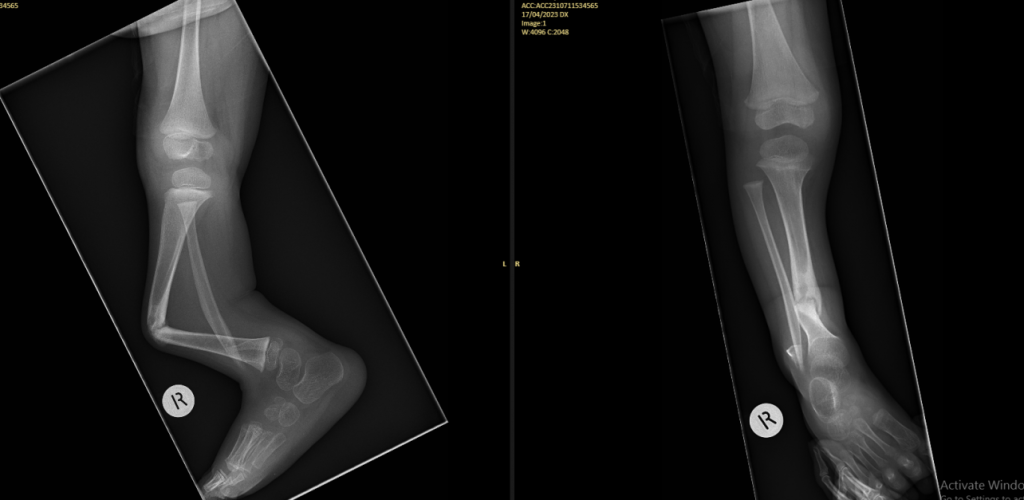
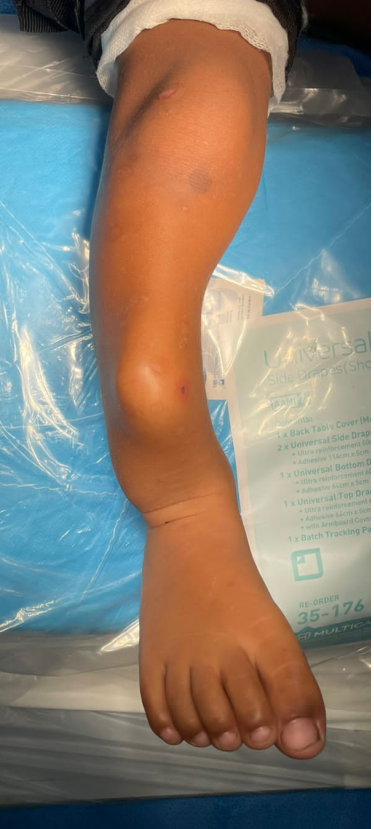
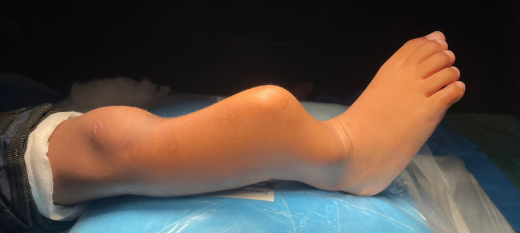
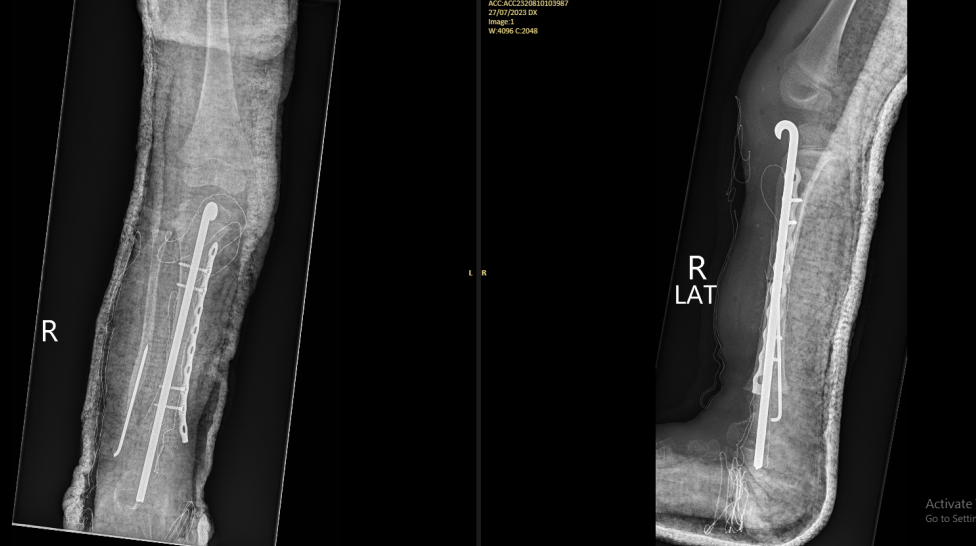
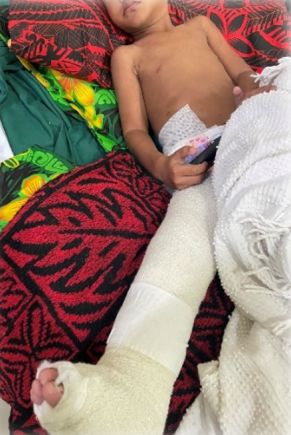
Both Tim and Jason Volunteered their precious time and expertise in coming to Samoa to perform surgeries for both these rare cases for free. Both Surgeons paid for their airfares and accommodation to travel for that week in Samoa.With all the cost involved for both these cases each case cost about 50,000-70,000NZD for each patient if they were to be transfer to NZ for this treatment and even more for other special services involved.This not only benefited our government but also building capacity for our local staff in knowledge and to operate on these rare cases. This was the biggest success of the visit for both families and also our health department especially moving forward to the future of developing specialized services on island.

First and foremost, we would like to thank team from New Zealand for the sacrifice they made while on holiday to operate on these surgeries. It goes without saying that their willingness and commitment to help us cater to the people of our country is remarkable and incomparable. They also managed to provide their own equipment that were used on their cases which was a huge help for us during our busy schedules in the theatre. The surgeries that were carried out are usually done overseas but having them performed on island made a huge impact on the lives of our patients and the services that we provide locally.To our local staff, thank you for showing up and being able to show enthusiasm to learn and grow in this profession. It is a milestone to witness and observe high skilled surgeons in action and I hope that we have each learnt a lot from this rewarding experience.Thank you also to Dr Faamuamua Arasi and Dr Cecelia B Vaai for working side by side with us in the past few weeks. Malo lava le tautua.And lastly, we’d like to acknowledge the Ministry of Health and Director General for the support and making sure that this visit took place so that we’re able to further our knowledge in a field that’s forever evolving every day in terms of surgical techniques and case management.

PIOA ran a safe surgical teams workshop in TTM Hospital on Saturday 25 March 2023
The workshop focussed on Situation analysis, Decision making, Communication and Teamwork. Here are some comments from those who attended.
RN Faatalaleleigafou Maliko / Junior theater Nurse.
RN Heaven Isaia / Senior Theater Nurse.
RN Filipi Keresoma/ Senior Theater Nurse.
Dr Cecilia Vaai Bartley / Anesthetic Registrar -final year trainee.
It was good also that it involved everyone like the scrub nurse & surgeons, and this helps us deal with issues that affect patient safety and how we can all work as a team
Dr. Haynes Rasin, Buka, Bougainville
The week was very informative for me. I appreciated a lot of new knowledge gained in this section.
An example, that there is a condition called Blount’s disease which is similar to rickets. However, have certain features that a characteristic of each and thus differentiates from the 2. In Rickets, there is diffuse bowing, but in Blount’s disease there proximal tibial deformity with medial beaking. Also cupping, fraying and metaphyseal splaying are present in Rickets but absent in Blount’s disease.

I also appreciate the knowledge to guide growth in children. The techniques involved which I think that if I can assist to do at least 2, I can confidently do them in our setting provided our theatre meets the requirements, eg. need for II. As the simple, basic plate and 2 screws for use can be readily ordered for such. The other new thing I learnt here was the presence of the bars that affect the bone growth and lengthening. Now I know how to identify the bars, also know the pathology they will cause. Perhaps, in the past I did see some of them but just passed them since I did not know what they signify.
I would have thought that perhaps, having the pediatric module for 7 days then having the exam on the following Monday morning would have given ample time for me to grasp the ideas and principles well before the exam.
I really appreciated the club feet talk. I used to have trouble understand the Pirani score and the serial casting methods that go with it. I now have better understanding at least to do the casting in the order required.
The correct method of application of a hip spica on a traction bed. Having the right equipment makes it easier to do the procedure.
So now the challenge is for me to submit proposals for 2 traction beds for our hospital, 1 for children and 1 for adults.
I sincerely thank the visiting lecturers for their time, effort and commitment to impart on us the paediatric orthopaedic knowledge.
Perhaps, an overseas attachment would reinforce further this knowledge as I would have the opportunity to observe, assist in such procedures and gain confidence in doing them.
Thank you
Haynes Rasin

The National University of Samoa graduation ceremony was held on 31 March 2023 in Apia. Two PIOA graduates Dr Areta Samuelu from Samoa nd Dr Pita Sovaonivalu from Fiji were awarded the Master of Surgery (Orthopaedics). It was a privilege for students attending the PIOA module in Samoa to be able to join in and observe the graduation ceremony. Dr Shaun Mauiliu, PIOA President and Dr Des Soares, Deputy Director of Training were also able to participate in the academic procession. PIOA is very grateful to Dr Rossana Pifeleti, Dean of the NUS School of Medicine for including us in the ceremony.
I am writing to express my utmost gratitude for the PIOA Paediatric Orthopaedics Module that I was a privileged to attend from the 13th to 18th of March 2023 in Apia, Samoa.

There were quite a number of new concepts taught that opened my eyes to how I should manage paediatric bone cases and I am greatly impressed and challenged to think beyond what I am used to seeing and practising in my country Papua New Guinea.
I am so pleased to learn that there is something we can offer to most of our patients whom we think nothing else can be done for. The most impressing concepts for me were:
– the cerebral palsy Gross Motor Function Classification System (GFMCS) that we can use to assess how as Orthopaedic surgeons, we can assist these children have a better quality of life when they grow up and become adults. It was interesting to see that they too can continue to be part of the productive work-force even if they’re GFMCS III. We surgeons play a role in helping the physicians manage cerebral palsy cases.
– the Osteomyelitis management emphasis on early diagnosis and drainage to save bone and reduce the unwise use of multiple antibiotics for long term therapy in osteomyelitis. This is so useful as I see a lot of these cases in my out-patient clinics and managing them is not always straight-forward.
– the calculation of LLD and the orthopaedic management options available for the children with LLD, how we can help save their limbs and prevent other skeletal deformities. This will lead to a better quality of life in the future and give them hope to find work and contribute to the country’s economic growth.
– the guided growth-plate arrest concept is also very useful and doable now that we have II in Port Moresby for those children with deformities from Blount Disease or Rickets condition.
– DDH screening is important early on and follow-up very useful so we can intervene early as surgeons and prevent major complications for the affected child’s development.
I look forward to more zoom classes and modules with PIOA that will help me expand my knowledge and skills in Orthopaedics so I can do better for my people around Papua New Guinea and the Pacific.
Editors note: PIOA is grateful to the Pacific Community and AO Alliance Foundation for their generous funding for this program.
The PIOA AGM 2023 was held online on Sunday 26 February 2023 commencing at 4pm AEST(Brisbane time).
Here are the papers from the meeting;
Draft Minutes of the AGM (to be ratified at next AGM in Feb 2024)
PIOA Trainee report – Raymond Saulep
Treasurer report – the Treasurer presented the Summary accounts and the Financial statement for PIOA Queensland Inc listed below.
Summary accounts (for all bank acounts)
The next PIOA module will be held at the Tupua Tamasese Meaole (TTM) Hospital in Apia, Samoa from 13 March to 1 April 2023. The topics covered will include Paediatric orthopaedics (13-18 March), Tumour (20-24 March), and Infection, Inflammation and Professional topics (25 March to 1 April).

We will have students from Timor Leste, Papua New Guinea, Solomon Islands, Fiji, Cook Islands, Samoa and American Samoa at the module. The module is sponsored by AO Alliance Foundation and the Pacific Community (SPC).
We will also celebrate the graduation ceremony from the National University of Samoa of our recent graduates Dr Areta Samuelu and Dr Pita Sovanivalu.

In his own words:
I’m currently working as acting Chief Medical officer in orthopaedics at Labasa Hospital (only divisional hospital in northern fiji serving a population of 150000).
Thanks to PIOA for what it has done for me in regards to :
Improve my theoretical orthopedic knowledge.
Taught me the importance of taking a proper history and examination.
Improve my surgical skills .
Continuous CME every Sunday.
Arranging individual mentoring with senior orthopaedic doctors from Australia/ NZ.
Provide a platform for discussion of cases and treatment plan.
Arranging for visitation of orthopedic team to our respective hospital to come and help in attending complex cases.
I hope and pray that PIOA will continue to do orthopaedic training in the Pacific.